1 Introduction: initial research that led to this practice insight
This practice insight is based on conclusions drawn from a research study conducted between 2017 and 2019. Funded by the Kettering Foundation based in Dayton, OH (US), 1 the study compared the effects of three communication-based community health interventions implemented in rural communities in a southern state in the United States. 2 The interventions aimed to motivate citizens to take individual or collective actions to address a pervasive public health issue: type 2 diabetes. 3
The interventions included: an expert speakers’ series comprising six hour-long presentations on topics related to diabetes, each followed by a question-and-answer session; a series of small group conversations based on the collective impact framework, led by trained facilitators; 4 and a deliberative discussion on the pros and cons of various community-based approaches to addressing diabetes, followed by a participant training on convening and hosting similar meetings.
The team initially defined intervention effectiveness as participants’ self-reported willingness to take individual or collective action to address diabetes following one of the three selected interventions. Evaluators also surveyed participants’ self-reported completion of these actions six months after the intervention. The team aimed to assess whether the method of convening community members influenced participants’ feelings of self- and collective efficacy when addressing a common chronic disease.
We also noted recent trends to move away from deficit models of science and health communication — i.e. experts imparting knowledge to an uninformed public — toward more participatory, dialogue-based models of engagement [See Trench, 2008 ]. By comparing the models, researchers hoped to pinpoint the public health benefits of creating a discursive space that recognizes and values participants’ lived experiences and community knowledge. 5 We predicted that the deliberative, democratic interventions would have a stronger association with self-reported individual and collective action related to the issue compared to interventions that relied on deficit models of science communication.
Overall, we conducted 45 community-based communication interventions, collecting over 100 hours of audio files and nearly 250 surveys.
Six-month follow-up interviews with event participants yielded disappointing results. Approximately 30 percent of participants reported taking some individual action, such as requesting an A1C test, starting an exercise program or making changes to diets, to address Type 2 diabetes, either for themselves or on behalf of a friend or family member. None of the interviewed participants reported engaging in any type of collective action, such as seeking information on how to conduct a community walkability assessment, exploring possibilities of joint use agreements with local schools to access tracks and gyms, or forming partnerships to start and maintain a community garden. 6
To analyze the discursive data, we used an iterative process. We transcribed audio tapes and coded transcripts individually. We then used a constant comparative method of coding and interpreting data by comparing new incidents to incidents already coded and categorized. We adjusted the conceptual possibilities through a series of weekly data sessions until we reached theoretical saturation. 7
While analyzing the qualitative data, we realized that the original research design may have been both too narrow and too ambitious. The team attributed this to two early methodological miscalculations. The first was underestimating the power of the dominant narrative of diabetes, one that posits the disease as a personal tragedy, best addressed through self-reliant health behaviors. The research team had assumed, incorrectly, that lay participants would be able to understand and apply a social ecological model of health behavior to their own experiences of diabetes, allowing them to explore community-level solutions as a group [See McLeroy et al., 1988 ]. This task proved difficult if not impossible, as participants continuously cited intrapersonal factors — rather than institutional or community-level factors — as the most essential elements of disease prevention and management. As such, the team agreed that any future pushes to reframe diabetes as a community health issue would first need to account for, if not attenuate, the preeminent, individualized order of diabetes discourse [Foucault, 1981 ]. 8
The design’s second miscalculation was the failure to consider community readiness — broadly defined as the motivating sum of a group’s topical literacy, community literacy, issue prioritization, and shared vision for the future — as a strong predictor of action on a science or health issue, be it individual or collective. This realization forms the basis of the practice insight presented here.
Based on this analysis, we argue:
- Engaging citizens in any type of communication-based health intervention requires first assessing a community’s readiness for action; and
- Community readiness — rather than communication method — is the better predictor of individual or collective actions, especially on public health and science issues.
2 Assessing community readiness for action: four primary determinants
As follow-up interviews revealed, none of the study participants reported taking any action to address Type 2 diabetes as a community. For the research team, this finding was particularly disappointing for communities that hosted facilitated meetings, an intervention that included a guided action planning process. In these cases, while the dominant, individualized narrative of diabetes management may have influenced the outcome, analysis of the discourse also revealed that we overestimated participants’ readiness to engage in collective action. Through thematic analysis of the transcripts from the facilitated conversations, we found that much of the talk focused on four underlying topics: practical skills to manage Type 2 diabetes; individual responsibility for health outcomes; consideration for peripheral community concerns; and uncertainty about the community’s future. Further analysis allowed us to dissect the discursive construction of community readiness, revealing four composite parts: issue alignment, issue literacy, community literacy, and visualized future (or valorized past). 9
2.1 First determinant: issue alignment
Issue alignment refers to the salience of an issue and the perceived urgency to address it compared to a community’s other identified concerns. Exemplars of participant statements indicating issue alignment — or, in many cases, issue mis alignment — included:
I am well aware that we have a very significant issue [with diabetes] in our area
…diabetes is such a prominent issue in our community and we need to see what we can do to help with it.
Jobs, that’s what they need most of all …We need jobs because every plant we had here has went but [names a plant] and they are not working this year.
What happened to housing is just …people when they moved and no one bought their house, they just sat there and they went down and nobody came.
High issue alignment is evident in the first two examples, where participants clearly perceived a sense of urgency regarding diabetes management. The third and fourth statements imply low issue alignment, suggesting that other issues — such as unemployment or abandoned property — warrant more attention than Type 2 diabetes. In communities with low issue alignment, residents may struggle to prioritize a single issue — especially if that issue is widely considered an individual concern, as is true with Type 2 diabetes. Thus, for this study, low issue alignment may have hindered participant consensus and, in turn, limited collaboration.
2.2 Second determinant: issue literacy
Issue literacy discourse aligns with one of two subcategories: a person or group’s practical understanding of a given issue and their perception of fellow community members’ knowledge of the same subject. For health topics, issue literacy parallels common conceptions of health literacy. In the present study, individual Type 2 diabetes management emerged as the central issue, regardless of any prompt to consider institutional or community-level determinants of health. Discursive constructions of issue literacy took several forms:
2.2.1 Exemplars of discourse related to participants’ issue literacy
I mean, you know, when I was diagnosed [my blood sugar] was 280. 10 It’s at now 200 now. But the way I’ve done that was cut out all my sugars, and exercise. Went with Splenda instead of sugar. And it’s probably not good for you, but you know, aspartame or whatever they say it causes cancer, causes all kinds of side effects, whatever.
We treated prediabetics for years with metformin. To help them, to keep them from, from becoming diabetic.
I’m actually doing the Vigo right now. Do you know what Vigo is? Vigo is one of the new ones. It’s like a pump. I get 40 units all day long and then I have the 36 units built it and it’s just a little box.
The first exemplar suggests the participant had low issue literacy regarding Type 2 diabetes. The participant equates replacing granulated sugar with artificial sweetener with “cutting out all [his] sugars.” This indicates an incomplete understanding of carbohydrate metabolism, namely an awareness that foods without added sugar can still raise blood sugar levels (e.g., potatoes, watermelons, and bananas). The second exemplar indicates the participant had a relatively high level of issue literacy, likely derived from their work as a healthcare professional. The third example demonstrates a participants’ grasp of their insulin regimen, though there is not enough information to determine the scope of their understanding.
2.2.2 Exemplars of discourse related to participants’ perceptions of community members’ issue literacy
A lot of people who come to me are totally confused. [The newly diagnosed diabetic patients] weren’t eating right in the first place; they have no idea what they’re doing.
The patients I have, they don’t understand the seriousness. They think you can just take a pill, not change your lifestyle, just increase your insulin, [without regard for] long term consequences, organ, kidney failure, heart disease, every organ in your body.
These excerpts capture participants’ perceptions that other community members — particularly those with diabetes — have low issue literacy regarding nutrition and disease management. Observations tended to come from clinician participants and reference patients with diagnosed Type 2 diabetes. This construction of community members with low issue literacy reinforced the order of diabetes talk, limiting the subject of diabetes to a personal realm rather than a public one; thus, prohibiting consideration of any type of collective action. Participants identifying as healthcare professionals drew implicit distinctions between the knowledgeable clinician and the ignorant or ill-informed public, a sign of ‘information deficit’ models at work.
2.3 Third determinant: community literacy
As with issue literacy, community literacy discourse tended to fall into two subcategories: resource awareness and resource coordination.
2.3.1 Exemplar of community literacy discourse related to resource awareness
Facilitator: so, you said Juvenile Diabetes Research Foundation [is a good community resource]. All right.
Participant 1: wait, but is that the camp that like [names a person] started? Do they have like an office here or where?
2.3.2 Exemplar of community literacy discourse related to resource awareness
Facilitator: what other groups do you most often think of?
Participant 1: girls and boys clubs kinda get the youth interested…
Participant 2: true. Someone came Friday and got material [from the community health clinic]. They were having something…Freedom for Youth. That’s a pretty big organization, I guess.
2.3.3 Exemplar of community literacy discourse related to resource awareness
Participant 1: I didn’t know we had all this, y’all may know we have, you may know we had the, have you heard of the Hound Café at the school? They have the Hound Café at this school. Did you know that they had that? A project of family and consumer science and it’s a cafe that is offered, operated as a business by the students.
Facilitator: is that their only cafeteria or do they have another one?
Participant 1: it’s public. The public can come there.
Participant 2: oh! We should have our coalition meeting there! That would be fun!
As these examples demonstrate, this subcategory of community literacy includes exchanges that deepen participants’ awareness of locally available resources, typically by exploring other participants’ social or professional connections. In essence, resources awareness is evident in true conversation. In the first exemplar, after one participant names a possible resource, another participant seems surprised that the organization is more than just a camp for children with Type 1 diabetes. The second exemplar suggests a discursive construction of resource awareness that builds from one participant’s vague reference to another’s more focused statement, though the second participant hesitates to add detail.
The third exemplar indicates a more sophisticated, well-developed sense of resource awareness, as the first participant describes a café that a local school runs as a business, and another participant suggests visiting the café as a group. The tenor of this exchange connotes more enthusiasm for finding and using new resources than the previous examples.
2.3.4 Exemplars of community literacy discourse related to resource coordination from four different community events
I mean, money is going to be one of your key factors for getting the community involved.
’Cause’ve you got the mayor and economic development. Those two are going to be our key players, and then if the mayor feels that we need to take something to city council — if he wants to broaden it out and make it bigger — then we could take it to city council.
We used to have, if you’re familiar with the Health Department, their hometown health coalitions. But I don’t think we… Ours is not active anymore, here.”
I would have to talk to [other community members] mostly at church or at exercise somewhere. You know, where I’m going because I don’t go a lot of places like I used to do, but I can tell them about things, you know, if, if they have place or whatever they had or how you work with certain areas, how it helps you to get you your diabetes down.
Resource coordination refers to participants’ knowledge of and access to processes or people that can effect change. The first two exemplars reflect participants’ understanding of social and political power in their community. The third example suggests an awareness that community health engagement has declined. The fourth quote is a self-assessment of a participant’s ability to influence health discourse through membership at local institutions, e.g., church.
The first three utterances position resource coordination as external to the participant group. Further, the resources referenced in the first and third excerpts are notably devoid of humanity. “Money” is the subject in the first exemplar; “the community” is the object. In the third, the faceless “Health Department” is the actor, and an impotent actor at that. Likewise, while the second exemplar names external entities — “the mayor” and “economic development” [in reference to city commissioners] — the participant still refers to the positions rather than the political actors. Unlike the preceding three, the fourth exemplar focuses on the participants’ perceived self-efficacy, a commentary on their power to coordinate resources. This is also the only exemplar that considers personal interaction as a viable means of effecting change.
2.4 Fourth determinant: visualized future vs. no visualized future or a valorized past
Visualized future refers to an ability to envision a different trajectory for the community. The counterpoint to visualized future talk is discourse that focuses on what was rather than what will be . This tendency to valorize the past creates a discursive world where a community’s best days are behind it. Discursive constructions related to visualized future (or valorized past) include the following:
2.4.1 Exemplar of visualized future discourse from an event in community in which the conversation focused on building partnerships to address public health issues
Maybe it isn’t about tying it to any kind of past success or history. It’s the idea of, the idea of building, as the partnership comes to be, then realizing ’what’s the story of how that happened?’ And then going back to this idea of this county. Then it’s telling that story, the story of how the community partnership happened, to show a new group of people how success might happen.
2.4.2 Exemplar of valorized past discourse from an event in a community that had experienced economic decline
We don’t have a movie theatre, we don’t have bowling. I remember when it was so many people here, stores was here. You could hardly walk down [the main street]. Now you got it all by yourself.
The visualized future example, above, is discourse that works to create a positive visualized future of cooperation and partnership, a future to be proud of. The valorized past exemplar focuses not on the future but on a glorified past, signaling a belief that the community’s best days are gone. Separately, our analysis also revealed that, in at least one community, the discourse included neither a visualized future nor a valorized past, suggesting little sense of community at all.
2.4.3 Sorting the relationships among the determinants of community readiness
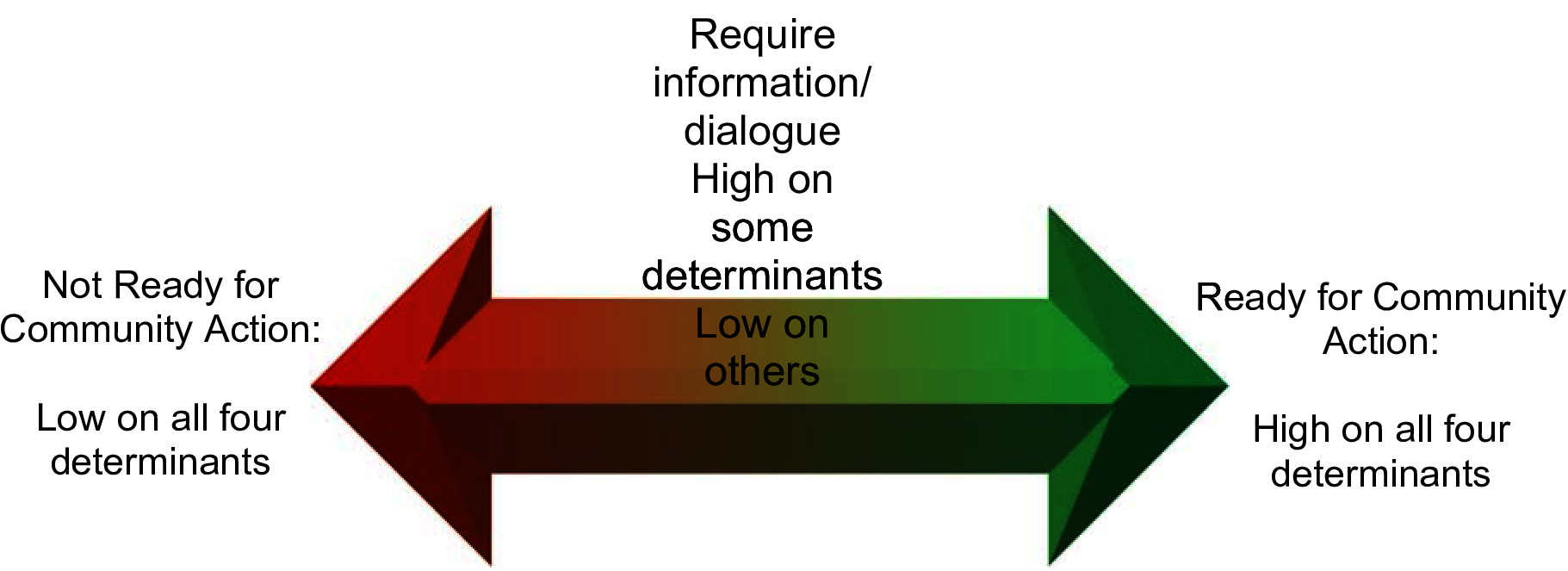
Our analysis of participants’ discourse suggests community readiness for collective action depends on the four interactive determinants identified above, which existed on a continuum as indicated in Figure 1 .
Optimum community readiness requires high issue alignment, high issue literacy, high community literacy, and a clearly visualized future. Our analysis of the discursive data from facilitated meetings suggests that none of the talk in any of the meetings worked to create a social world where participants were ready to address Type 2 diabetes as a community health issue. On the other hand, in all communities except one, the talk suggested some degree of individual readiness to engage the issue of diabetes, although at disparate stages and in different ways.
Assessing community readiness for action, then, is the first step to meaningful community engagement. However, this raises two key questions for science communicators: 1) What work must science communicators do to assess community readiness for action? And 2) How can science communicators adapt engagement strategies based on a community’s assessed readiness?
3 Assessing community readiness for action: community analysis and communication strategy development
3.1 Community analysis beyond demographics and general attitudes
Science communicators are well aware that audience analysis is a critical component of any successful communication interventions. However, we often limit these analyses to an understanding of sociodemographic segmentations within communities, individuals’ general attitudes toward the issue under discussion, and how individuals search for and consume information about specific public health or science issues [See e.g., Metag and Schäfer, 2018 ]. These are excellent starting points for understanding two of the determinants of community readiness for action: Issue Literacy and Issue Alignment . Still, we find that science communicators rarely consider their audience’s level of Community Literacy or general orientation toward a Visualized Future versus a Valorized Past .
Documenting a group’s Community Literacy and Visualized Future is possible using common field research methods, such as short surveys or focus group discussions. Practically speaking, our team inadvertently convened focus groups about community readiness for health action — we simply did not realize it at the time. The community conversations generated valuable insight for planning future community health interventions related to diabetes, especially those targeting institutional or community-level determinants of health. Taking the time to expand standard audience analyses will provide science communicators with a more holistic, more realistic assessment of a community’s ability to address science and health issues collaboratively. This expanded assessment also promises to equip science communicators with important baseline data for determining an intervention’s ultimate effectiveness, allowing for evidence-based public health and science practices.
3.2 Designing effective communication intervention strategies
Assessing a community’s readiness to act on any public health or science issue is essential for working with communities to design effective ways to communicate about and act on that issue. As science communicators, it is essential that we meet communities where they are at — not where we want them to be.
We encourage science communicators to dignify and respect their community partners by first assessing their readiness for proposed action and then working with communities to determine appropriate methods of engagement. The progressive step model (Figure 2 ) suggests interventions based on level of readiness. 11
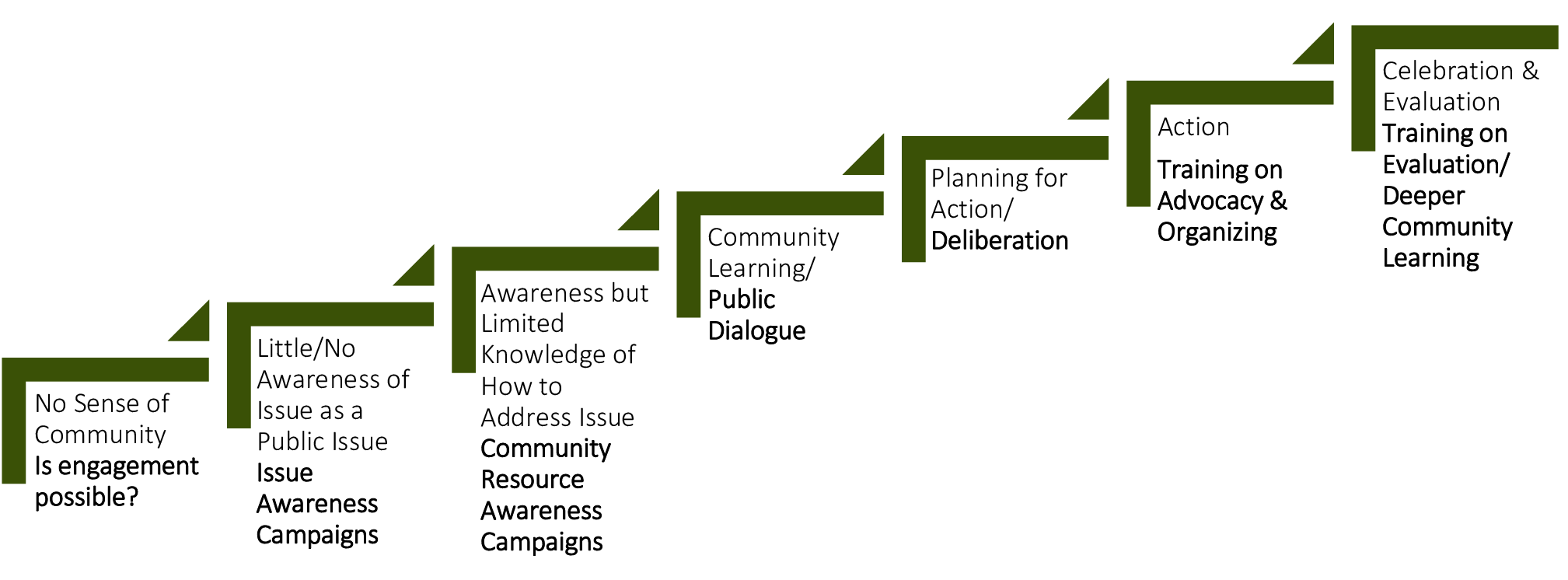
There are many things worth noting about the proposed model, four of which we mention here. First, the lowest (or earliest) level of community readiness pushes practitioners to consider that, when a community scores low in all four determinants, traditional engagement may not be possible. The model implies that a sense of community is a prerequisite to providing a discursive, deliberative space for science communication. Without that sense of community, science communicators’ attempts to facilitate action may be met with silence at best and hostility at worst.
Second, the model’s second and third tiers exemplify what Trench [ 2008 ] termed a deficit model of science communication, matching this approach to communities with low issue awareness or low awareness of community resources. Rather than driving a wedge between science communicators and community members, community-centered awareness campaigns may bring scientists and community members to better understandings of each other, laying the groundwork for common understanding and illuminating opportunities for collaboration. In fact, helping communities reach higher levels of potential engagement may first require culturally appropriate distribution of information. This applies most to complicated topics that garner public interest, where community members would need a technical understanding of the issue in order to fully and meaningfully explore possible solutions.
Third, the model’s fourth tier proposes that a community’s ability to discuss an issue is a precursor to deliberating ways to improve or solve that issue. Much has been written about the relationship between dialogue and deliberation. 12 Often, deliberation theorists and practitioners operate from the assumption that if people have enough accurate information about a topic, then they can deliberate how to address it without complication. In turn, various theorists and practitioners have questioned the assumption inherent in deliberative theory, that when people deliberate, they come to reasoned decisions. For example, at a recent National Coalition for Dialogue and Deliberation (NCDD) conference, much discussion focused on the need for citizens to explore their emotional connection to issues before engaging in deliberation. 13
Moreover, offering opportunities for community members to engage in dialogue before moving to deliberation creates a social world in which public discussion is considered a culturally normal (if not reliably beneficial) practice. In short, we argue that dialogue before deliberation leads to common understandings about complicated public issues and, eventually, to more authentic and productive deliberation.
Finally, the top two rungs of the model suggest science communicators have a duty to work with communities that are ready to act on a public health or science issue to engage community members in designing effective and appropriate methods of advocacy, organizing and evaluation of actions taken. The work does not stop with decisions concerning how to frame the issue or how to set the public agenda on the issue; the work continues with carrying out that agenda.
4 Conclusion
We have argued that engaging citizens in any type of communication related to public health or science requires first assessing a community’s readiness for that action. Further, we submit that community readiness — rather than communication method — is the better predictor of individual or collective action on a health or science issue. Admittedly, the study’s practical implications may seem limited by the small regional participant sample. Our analysis and discussion are based on one research study, which focused on encouraging rural communities in a Southern U.S. state to address Type 2 diabetes.
However, we suggest the determinants of community readiness and the presented model have implications beyond the geographic area in which we worked and the public health issue we addressed. We argue that science and health communicators could use these tools to design tailored public information campaigns around a variety of topics, such as the COVID-19 pandemic, the spread of seasonal influenza, or even climate change. This could lead not only to more citizen engagement with these issues, but to more productive engagement that focuses on systemic change rather than individual behavior modification.
Further, we hypothesize that our findings would ring true in other contexts, and we argue that each model offers useful perspectives for public health practitioners and science communicators. To our fellow researchers and practitioners, we welcome feedback and collaboration in the interest of finding better ways to engage communities not only in discussing public health and science issues but in working with public health practitioners and scientists to act on those issues in effective and democratic ways.
References
-
Bennett, J. A. (2012). ‘Troubled Interventions: Public Policy, Vectors of Disease, and the Rhetoric of Diabetes Management’. Journal of Medical Humanities 34 (1), pp. 15–32. https://doi.org/10.1007/s10912-012-9198-0 .
-
Coleman, J. S. (1988). ‘Social Capital in the Creation of Human Capital’. American Journal of Sociology 94, S95–S120. https://doi.org/10.1086/228943 .
-
Escobar, O. (2009). ‘The dialogic turn: Dialogue for deliberation’. In-Spire Journal of Law 4 (2), pp. 42–70.
-
— (2011). Public dialogue and deliberation: A communication perspective for public engagement practitioners. Edinburgh, U.K.: Beacons for Public Engagement.
-
Foucault, M. (1981). ‘The order of discourse: Inaugural lecture at the College de France’. In: Untying the text: A post-structural reader. Ed. by R. Young. Original work published 1970. Boston, MA, U.S.A.: Routledge, pp. 51–78.
-
Glaser, B. G. (1965). ‘The constant comparative method of qualitative analysis’. Social Problems 12 (4), pp. 436–445. https://doi.org/10.2307/798843 .
-
McLeroy, K. R., Bibeau, D., Steckler, A. and Glanz, K. (1988). ‘An Ecological Perspective on Health Promotion Programs’. Health Education Quarterly 15 (4), pp. 351–377. https://doi.org/10.1177/109019818801500401 .
-
Metag, J. and Schäfer, M. S. (2018). ‘Audience segments in environmental and science communication: recent findings and future perspectives’. Environmental Communication 12 (8), pp. 995–1004. https://doi.org/10.1080/17524032.2018.1521542 .
-
Prochaska, J. O. and DiClemente, C. C. (1992). ‘Stages of change in the modification of problem behaviors’. Program Behavior Modification 28, pp. 183–218.
-
Trench, B. (2008). ‘Towards an analytical framework of science communication models’. In: Communicating Science in Social Contexts. New models, new practices. Ed. by D. Cheng, M. Claessens, T. Gascoigne, J. Metcalfe, B. Schiele and S. Shi. Dordrecht, Netherlands: Springer, pp. 119–135. https://doi.org/10.1007/978-1-4020-8598-7_7 .
Authors
Christina Standerfer, Professor Emerita, University of Arkansas Clinton School of Public Service, earned a PhD in Communication from the University of Colorado. Her work centers on the importance of understanding the role of public discourse in facilitating social justice and citizen participation in developing responsive and ethical public policy. E-mail: ccstanderfer@clintonschool.uasys.edu .
Emily Loker, PhD candidate in the communication department at the University of Colorado Boulder, works at the intersections of communication, activism for social justice, pedagogy, and community-based research. She earned her master’s in Public Service from the Clinton School of Public Service and is a two-time AmeriCorps alumna. E-mail: emily.loker@colorado.edu .
Jason Lochmann earned a Master of Public Service from the University of Arkansas Clinton School of Public Service and a Master of Public Health from the University of Arkansas for Medical Sciences. He now works as a Communications Specialist for the Louisiana Public Health Institute, specializing in maternal and child health projects, as well as data-based suicide prevention messaging. E-mail: jason.lochmann@outlook.com .
Endnotes
1 The Kettering Foundation is a nonprofit organization rooted in the tradition of cooperative research that is conducted from the perspective of citizens and focuses on what people can do collectively to address problems affecting their lives, their communities, and their nation. https://www.kettering.org/about .
2 In collaboration with the state department of health, we identified 15 communities to participate in the study: three from each of the five public health regions in the state. Selection was based on similarities in population, demographics, and relatively high rates of diabetes. In regard to educational levels beyond high school, median income, and percentage of population living in poverty, the statistics of these communities mirrored state statistics in general, which ranks near the bottom on all three indicators: 47 (out of 50) in population with education beyond high school; 48 in median income; and 46 in people living in poverty. For more information see, America’s Health Rankings: Diabetes in the United States. Available: https://www.americashealthrankings.org/explore/annual/measure/Diabetes and https://www.census.gov/quickfacts/fact/table/AR,US/PST045219 .
3 We chose to focus on Type 2 diabetes for two reasons: 1) our previous work with the state health department to investigate best practices for engaging communities in curbing rates of the disease; and 2) the Kettering Foundation’s interest in investigating how public health policies could be democratized through community dialogue. Admittedly, framing diabetes as a public health issue may have been a tall task to begin with. However, Jeffrey Bennett [ 2012 ] argues that the mission of public health is increasingly situated “in the realm of noncommunicable disease” although public health infrastructure has not kept pace with the shift from communicable to noncommunicable diseases. He further argues that moving the policy debate regarding diabetes away from individual self-management to issues of systemic intervention requires a public reframe of the disease as an “epidemic” as the term implies a need for political and public action beyond individual self-management of the disease.
4 For more information on this model see, National Council of Nonprofits: Collective Impact , https://www.councilofnonprofits.org/tools-resources/collective-impact .
5 We are building on Coleman’s [ 1988 ] definition of social capital here. Coleman notes, “social capital is defined by its function. It is not a single entity but a variety of different entities, with two elements in common: they all consist of some aspect of social structures, and they facilitate certain actions…” Unlike other forms of capital, social capital inheres in the structure of relations between and among actors . It is lodged neither in the actors themselves or in physical implement of production” (p. 98, emphasis added). For more information, see Coleman [ 1988 ]
6 Information on how the state health department could provide technical support for collective action was distributed at all community events.
7 For more on the constant comparative methods, see Glaser [ 1965 ].
8 Foucault noted discourses are more than vehicles for conveying preexisting meaning: “they have a ponderous, formidable materiality.” Discourses order us to think and act in certain ways. We can become trapped in our discourses in ways that do not allow new perceptions of what we hold to be true, and these truths are often received from those a society deems to be experts. Few fields have such a clear distinction between expert and non-expert as medicine.
9 Through our data analysis, we realized how complicated community readiness is. Our search for literature related to the term yielded one model, the Community Readiness Model (CRM), that had been used in a handful of studies related to obesity but none related to diabetes. This model was developed at Colorado State University and includes five key dimensions and nine stages of community readiness. CRM was developed by combining two existing theoretical models: Prochaska and DiClemente’s Transtheoretical Model of Individual Behavior Change and Warren’s social action process for community development. In contrast to this theory driven deductive approach, the model we present here was developed using an inductive approach starting with discursive constructions of community members. See Community Readiness for Community Change available: https://tec.colostate.edu/wp-content/uploads/2018/04/CR_Handbook_8-3-15.pdf .
10 For comparison, blood sugar levels less than 99mg/dL are considered normal.
11 This model is similar to Prochaska and DiClemente’s [ 1992 ] Transtheoretical Model of Behavior Change, which posits five stages individuals move through to adopt a new way (presumed better or healthier) of acting: Pre-Contemplation, Contemplation, Preparation, Action, Maintenance and (perhaps) Relapse [Prochaska and DiClemente, 1992 ].
12 For reviews of the various theoretical groundings of both dialogue and deliberation, see Escobar [ 2009 ] and Escobar [ 2011 ].
13 For more information on NCDD see https://ncdd.org .